Document Type : Original Research Article
Authors
1 Department of Chemistry, Payame Noor University, P.O. BOX 3149968143, Karaj, Iran
2 Research Center Karaj Moallem, Karaj, Iran
Abstract
Breast cancer is one of the most common cancers and a large number of breast surgeries are performed every year. Most of these surgeries require the use of breast three dimensions (3D) prostheses and implants or drug-containing scaffolds. In most cases, prostheses and scaffolds are made of organic and inorganic materials which are not biocompatible. Using plant tissues and fibers instead of these materials to make 3D prostheses and scaffolds that naturally contain anti-cancer drugs is a new idea that has gained attention in recent decades. Recently, the radiation of infrared light (IR) waves to the organ containing the drug-carrying 3D prosthesis has been used to release the desired amount of drug from prosthesis at the desired time after surgery. The IR radiation is introduced as the fourth dimension in the 4D prosthesis and is a newer idea. In this research, the ultrasound waves have been proposed as a fourth dimension for drug release and turmeric rhizome as a scaffold containing curcumin as an anti-cancer substance. The process of releasing the curcumin from the turmeric rhizome - as a scaffold - with ultrasonic waves is a new and innovative idea that is in line with the development of 4D prosthetics.
Graphical Abstract
Keywords
Main Subjects
Introduction
Breast is the second most common cancer worldwide, especially among women. Despite preventive policies such as screening mammography, visualization, and palpation, breast cancer is often diagnosed late, leading to high mortality. In fact, according to the World Health Organization (WHO), in 2020, about 2.3 million women in the world were diagnosed with breast cancer and about 30% died. Survivors of this disease often need reconstructive prostheses due to the loss of part or all of their breasts. They also need drug-containing scaffolds as a kind of implant due to the possibility of disease returning [1, 2].
In 1955, Pangman prepared two-layer prosthesis with poly-plastic material and implanted it in the breast of a volunteer with limited facilities at that time. In 1963, an implant made of polyethylene strips with a length of about 2 mm was made in Turkey and placed in a patient's breast [3-6].
Due to the problems that plastic and polyethylene prostheses caused for the patient, these materials were gradually replaced with other materials compatible with the body. From 1966 onwards, silicone gel prostheses were used. These silicone prostheses received serious attention due to the higher patient satisfaction and fewer complications and gradually evolved [4-6].
However, the demand for the other types of prostheses, including scaffold prostheses, which require a stronger structure and sometimes multiple layers for drug loading, requires the use of other materials to prepare this new type of prosthesis. One of the important applications of scaffold prostheses is to use them to load anti-cancer drugs into cancer-prone areas [7-12].
In this treatment method, after the lumpectomy surgery, a scaffold implant containing anti-cancer drugs is placed in the breast so that the drug inside the scaffold is gradually released on the spot and destroys the remaining or produced cancer cells without need to new surgery. In addition, Chhaya et al. (2016) placed a scaffold made of polycaprolactone (PCL) containing a drug into the breast of small pigs [1].
In 2020, Wei prepared scaffolds using 3D printing prosthesis in which the drug anthracycline doxorubicin (DOX) in the capsulated form was loaded on it. This scaffold was implanted in the breast and after surgery at desired intervals, the breast was exposed to near infrared (near IR) radiation to destroy the capsule shell, which was made of polydopamine (PDA), and the DOX drug was released in the area prone to cancer recurrence [1].
This method, which considers a new dimension for Near-IR radiation, along with scaffold prostheses containing encapsulated medicine are known as 4D prostheses. In this way, in addition to destroy the shells of the capsules and releasing the anti-cancer drug, the radiation leads to a photothermic effect. Therefore, parallel to the drug’s effect, the photothermic effect also destroys cancer cells [1].
In addition to these chemical materials, the use of natural plant or animal-based materials in the manufacture of scaffold prostheses can have better results due to biocompatibility. Turmeric rhizome, which can be used mostly as an edible spice, has found a place in pharmaceuticals due to the recognition of medicinal properties of its active ingredient curcumin. Curcumin has been showed anti-inflammatory, antioxidant, and even anti-cancer effects [8, 13].
Curcumin is an organic substance with the formula C21H20O6, which can be seen in both ketone and enol forms, and of course it is mostly in the ketone form [10-14].
Laboratory research shows that curcumin has anti-cancer properties, preventing the spread of cancer, making chemotherapy more effective, and protecting healthy cells from radiation damage. Of course, the study of curcumin effect on humans is still in the early stages [8].
In the last few decades, extensive work has been done to understand the properties of curcumin and proven that curcumin has antioxidant, anti-mutagenic, anti-diabetic, antibacterial, hepatoprotective, expectorant, and anti-cancer medicinal properties [14-17 ].
The microscopic structure of turmeric rhizome shows a structure with high strength and scaffolding model. This property in turmeric rhizome with its active ingredient, curcumin, is a natural model of scaffold prostheses in which the drug is loaded on it. Therefore, it seems that this natural scaffold can be used instead of artificial models. Although many studies have been conducted on curcumin and the structure of turmeric rhizome, so far turmeric rhizome has not been used or even proposed as a natural scaffold model. This article discusses a new use for turmeric rhizome that contains curcumin [8-13].
When dealing with drug-carrying scaffold prostheses, the problem that exists and should be resolved is the release of a certain amount of drug in breast containing scaffold prosthesis at each stage. A part of the breast may need more medicine and a part may not need medicine at all. All these cases require a tool to control the release of drug from the scaffold, which was mentioned as the fourth dimension earlier [13,14].
For this purpose, the introduction of the fourth dimension has led to an increase in the complexity degree in prostheses. In fact, 4D prosthesis is still in its infancy [1].
In the 4D prosthesis, a series of waves (Near-IR) or stimuli are radiated from the outside of the body to the breast, stimulating the scaffold and leads to the release of a certain amount of drug inside breast [1-6].
No report has been seen about the use of ultrasonic wave stimulation as the fourth dimension in 4D scaffold prostheses. In this aspect, this article presents a new idea in using ultrasound waves as the fourth dimension in 4D scaffold prostheses which along with the suggestion of using turmeric rhizome as a natural scaffold, can be an attractive and innovative idea.
Experimental
Research variables
The variables include investigating the structure of turmeric rhizome for usability as a scaffolding prosthesis, investigating the effects of ultrasonic waves on the curcumin release from turmeric rhizome. The amount of curcumin released from the rhizome under ultrasonic waves and quantitative studies have been performed with the UV-Vis spectroscopy. Ethanol was used as solvent of curcumin due to the sufficient solubility of curcumin in ethanol. The investigated sample includes alcoholic solution containing turmeric rhizome exposed to the ultrasonic waves for different periods. The investigated parameter is the effect of ultrasonic irradiation time on the release of curcumin. The statistical population of this research includes 6 samples of alcoholic solution containing curcumin extracted from the alcoholic solution containing rhizome under ultrasound radiation in a certain period of time.
Materials and methods
The materials used in this research include curcuma tablets, turmeric rhizome ethyl alcohol, and distilled water. The laboratory equipment used includes ultrasonic bath model vCLEAN1-L13 with a voltage of 220 V and 50 Hz as a source of ultrasonic radiation, spectrophotometer (UV-Vis) model NDNM96, all made in Iran and optical microscope model: AC85-240V made in Japan.
Extraction of curcumin from rhizome
At this stage, 0.5 g of a piece of chopped rhizome was weighed and placed in a 500 mL beaker. Then 100 mL of ethyl alcohol was poured on the rhizome. As soon as the alcohol was poured on the rhizome, the color of solution turned yellow, indicating the rapid dissolution of curcumin in the alcohol.
To investigate the further dissolution of curcumin, the mixture of alcohol and rhizome was subjected to the ultrasonic radiation in the ultrasonic bath. The idea of conducting this research was that if some curcumin is trapped inside rhizome and has not yet dissolved in alcohol, by applying the ultrasonic radiation that creates high local pressure and temperature, the trapped curcumin inside rhizome fibers.
Ultrasonic radiation for curcumin extraction
According to Table 1, pure alcohol ethanol was selected as the reference, and then 0.5 g of chopped rhizome was poured into 100 ml of pure alcohol, which immediately changed to yellow color, which is a sign of dissolution of curcumin in alcohol.
After 10 minutes, when the color remained constant, 2 mL of the yellow alcoholic solution was removed with a pipette and poured into the control container before the ultrasound waves were radiated. In the following, the mixture of rhizome and alcohol was subjected to ultrasonic radiation for 5 min, and 2 mL of the yellow alcoholic solution was removed with pipette per minute and poured into a container labeled samples 1 to 5.
Finally, in a separate examination, the curcuma tablet powder was dissolved in 100 mL alcoholic solution and 2 ml of it was poured into the container of sample 6 to be compared with of the samples 1-5. The aim is to see if, by changing the ultrasonic time, more curcumin can be released from the rhizome into the alcohol until the curcumin substance in the solution is equivalent to the amount of substance obtained by dissolving one unit of curcumin tablet.
Results and Discussion
Microscopic studies
Figure 1a displays turmeric rhizomes. In Figure 1b and c, microscopic images of turmeric rhizomes are shown, adapted from Jia and Wang's research paper published in 2015 [9]. This structural model of turmeric rhizome is in good agreement with the synthetic scaffold model prepared by Chhaya [10], as depicted in Figure 1d. In this way, it may be possible to replace natural scaffolds of plant and animal origin instead of artificial and chemical scaffolds.
Due to its organic nature, turmeric rhizome can better adapt to the human body as a scaffold. For this purpose, turmeric rhizome was prepared and after grinding in a mortar, its powder was examined under a microscope.
Table 1. Characteristics of samples containing curcumin under ultrasound radiation
|
Samples under test |
Label |
Ultrasonic time/min |
|
Alcohol alone |
Reference |
0 |
|
Alcohol + curcumin |
Control sample |
0 |
|
Alcohol +curcumin |
Sample1 |
1 |
|
Alcohol + curcumin |
Sample2 |
2 |
|
Alcohol + curcumin |
Sample3 |
3 |
|
Alcohol + curcumin |
Sample4 |
4 |
|
Alcohol + curcumin |
Sample5 |
5 |
|
Alcohol + curcumin (tablet) |
Sample6 |
0 |

Figure 1. (a) Turmeric rhizome, (b) and (c) microscopic image of turmeric rhizome with different magnifications [9], and (d) scaffold prosthesis [10].
Microscopic images of the rhizome in Figure 2 illustrate hexagonal structures with an interesting resemblance to the structure of honeycomb and beeswax. Accordingly, this model can be used in the preparation of honeycomb scaffolds containing medicinal substances. Curcumin has been used as a medicine for many years. For instance, curcumin is used as a drug in Alzheimer's treatment [11, 12]. However, what is discussed in this article is the use of curcumin along with turmeric rhizome. In a way, the rhizome acts as a prosthetic scaffold and curcumin acts as a loaded drug that is naturally trapped in the honeycomb spaces and can be released by the external stimulation.
Effect of ultrasonic of curcumin extraction
The UV-Vis spectroscopic of the curcumin has been carried out in organic solution, as well as in aqueous solution. Since curcumin contains two types of ketone and enol, there is a hydrogen bond between these two types, which leads to the formation of a common conjugated chromophore, and the organic solution of curcumin shows a bright yellow color [8-15].
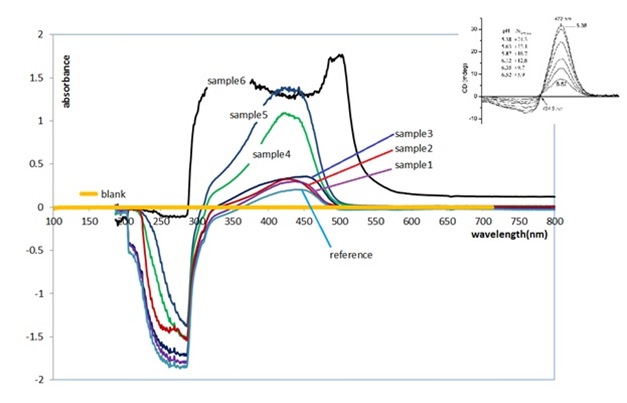
According to Figure 3 (upper right), the organic curcumin solution has a strong absorption peak at 427.5 nm and its absorption intensity changes slightly with different acidity. The highest absorption is at pH=5.95 [12].
The UV-Vis spectrometry of the samples (Table1) indicates alcohol ethanol as a reference has no absorption in the range of 200 to 700 nm. The control sample, which is an alcoholic solution of curcumin before ultrasonic irradiation, shows a weak absorption value in the range of 350 to 500 nm with an absorption peak at 427 nm. In the high-energy region below 350 nm, the negative absorption is observed, which is similar to what was observed in Zsila [11] and inserted in the upper right of Figure 3. This negative absorption is related to the cotton effect, which is out of our discussion [11].
By applying ultrasonic waves to the alcoholic solution containing rhizome from 1 to 5 minutes, the amount of absorption increases, which indicates the curcumin increase in the solution. The absorption spectrum of sample 6 related to the saturated alcoholic solution of curcuma tablets has a broad absorption peak with a saddle-shaped depression related to the overlap of two peaks of ketone and enolic curcumin, which is together with other available fillers. In curcuma tablets, it gives such a special spectrum. The constant position of the peaks in spectrum and the direct relationship of absorption with the increase in ultrasound radiation time, which shows the increase in absorption, show the repeatability and accuracy of the test.

Figure 2. Microscopic images of the honeycomb structure of rhizome and thread-like fibers inside it
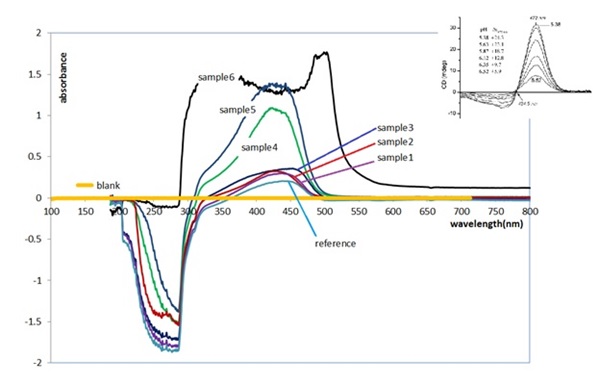
Figure 3. The UV-Vis spectrums of samples containing curcumin, inserted figure in the upper right is adapted from [11]
the widest absorption range compared with samples 1 to 5, but in terms of the height of the peak, its height is lower than that of sample 5, which was exposed to radiation for 5 minutes. These results show the fact that with 5 minutes of irradiation, the amount of curcumin released from 0.5 grams of turmeric rhizome is equivalent to the amount of curcumin in one unit of curcuma tablet. Therefore, the use of ultrasonic waves effectively increases the curcumin concentration in the solution.
Experiments show that with 5 minutes of ultrasonic radiation to a solution containing rhizome, the curcumin concentration in the containing solution increases and becomes equivalent to one unit of curcuma tablet. Using these results, a four-dimensional scaffold prosthesis based on turmeric rhizome can be designed, the fourth dimension of which is ultrasound radiation, and curcumin dose is increased as needed.
Analysis of ultrasonic effect on turmeric rhizome
In an inelastic medium such as water and most liquids, there is continuous wave transmission of sound, provided that the sound amplitude is relatively small. As the amplitude increases, as a result of the wave separation on the surface of liquid, microbubbles are created, which is called cavitation. In other words, to create cavitation bubbles, a pressure wave with high intensity and sufficient amplitude must pass through the liquid, which eventually causes the bubbles to burst, which release their energy in the form of sound waves locally and explosively. The accumulation and explosion of millions of bubbles in an ultrasonically excited liquid can produce temperatures of about 5,000 degrees Kelvin, pressures of about 1,000 atmospheres, and microjet velocities of 250 mph in the blast regions of cavitation holes. Therefore, according to this process, in the test of alcoholic solution containing turmeric rhizome, ultrasonic waves release a lot of energy in the solution, which results in the release of curcumin from the honeycomb structure of turmeric rhizome.
Conclusion
Scaffold prostheses containing anti-cancer substances are a new method to control recurrent cancers. Various materials are used to prepare the scaffold, which has the maximum strength and biocompatibility with the biological area. Replacing these materials with plant biological materials is a new and unique idea that few people in the world have followed. According to this research, turmeric rhizome can be used instead of chemical scaffolds due to its structural similarity. It contains the anti-cancer drug curcumin, which can prevent the development of breast cancer. For this purpose, the desired amount of curcumin can be removed from the rhizome and entered into the cancerous tissue using the ultrasonic radiation.
Acknowledgments
The authors would like to sincerely thank all those who provided them with the laboratory results. They would like to thank the student research of Moallem for providing them with laboratory space. The authors are grateful to those who gave spiritual support and would like to thank Tina's parents who sincerely and enthusiastically helped reach the goals of the research.
Disclosure Statement
No potential conflict of interest was reported by the authors.
Funding
This research did not receive any specific grant from funding agencies in the public, commercial, or not-for-profit sectors.
Authors' Contributions
All authors contributed to data analysis, drafting, and revising of the paper and agreed to be responsible for all the aspects of this work.
Orcid
Ashraf Heidaripour
https://orcid.org/0000-0003-0223-5383
How to cite this manuscript: Ashraf Heidaripour*, Tina Barati. Extraction of Curcumin by Ultrasonic Waves from Turmeric Rhizome as a Scaffold in 4D Prosthesis. Asian Journal of Green Chemistry, 7(3) 2023, 199-207. DOI: 10.22034/ajgc.2023.393836.1383